TEETH: CANARIES IN THE MINE?
What if dentists approached findings that indicate an imbalance in the mouth as a far more serious warning sign, like canaries dying in yesteryears mines?
What if dentists approached findings that indicate an imbalance in the mouth as a far more serious warning sign, like canaries dying in yesteryears mines?
Why do our attempts to deal with the challenges of our time so often fail? Why are we stuck in so many quagmires today? The cause of our collective failure is that we are blind to the deeper dimension of leadership and transformational change. This “blind spot” exists not only in our collective leadership but
Evidence indicates that poor maternal oral health can have significant consequences for a woman’s systemic health and that of her children. Similarly, transmission of oral bacteria from mother to child is well-documented and poses a risk for the development of early childhood caries, the most common chronic disease of childhood. Untreated maternal dental disease nearly
Paul Pholeros and his colleagues have been working for decades on improving health by improving the living environment and housing of Indigenous people in Australia. This successful model is now spreading to other continents. Ever since I watched this TEDx Talk, I have been wondering how we, dentists could apply similar thinking to improve health
Progress in dentistry has an intense focus on technology. And what more exciting for a dentist than a new high-tech instrument? I know. I used to say that the one who dies with the most toys wins. I was going to win this game. Early adopter across the board here! But is high-tech better? In some instances it surely is. When our patients come to the point of needing restorations, the technology that provides the best margins will benefit them for sure. But could there be better ways of benefitting our patients? This article was first published in the March 2013 issue of TEAM WORK, a Palmeri Publication.
The evidence connecting oral health to overall health continues to grow, and this is leading to changes in the way both dental and medical professional approach the care they provide to patients. When the root cause of health problems can be addressed, patients experience better outcomes and healthier lives. However, for this new approach to

Measuring oral health is difficult. Treating dental disease is challenging, labor intensive and extremely expensive. The currently accepted surgical approach to caries fails often and regularly and has a questionable return on investment…
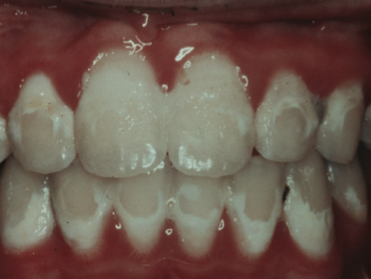
Orthodontic-Related Decalcifications & Caries from Dr Marielle Pariseau Decay risk exists for all patients to varying degrees in occlusal pits and fissures, interproximal surfaces and facial surfaces. Orthodontic treatment increases the risk of decay for a variety of reasons. Oral hygiene is more difficult; wires are in place for two to three years or longer

Are you frustrated that the (oral) health instructions given at dental exams rarely seem to result in positive change?
Do you feel you work harder at achieving good oral health for some of your patients than the patient does?
FInd out how Motivational Interviewing can help you help your patients.

Progress in dentistry has an intense focus on technology. And what more exciting for a dentist than a new high-tech instrument? I know. I used to say that the one who dies with the most toys wins. I was going to win this game. Early adopter across the board here! But is high-tech better? In some instances it surely is. When our patients come to the point of needing restorations, the technology that provides the best margins will benefit them for sure. But could there be better ways of benefitting our patients? This article was first published in the March 2013 issue of TEAM WORK, a Palmeri Publication.

What if dentists approached findings that indicate an imbalance in the mouth as a far more serious warning sign, like canaries dying in yesteryears mines?
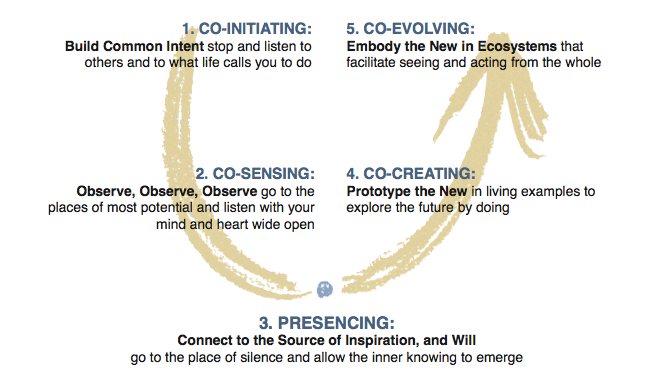
Why do our attempts to deal with the challenges of our time so often fail? Why are we stuck in so many quagmires today? The cause of our collective failure is that we are blind to the deeper dimension of leadership and transformational change. This “blind spot” exists not only in our collective leadership but

Evidence indicates that poor maternal oral health can have significant consequences for a woman’s systemic health and that of her children. Similarly, transmission of oral bacteria from mother to child is well-documented and poses a risk for the development of early childhood caries, the most common chronic disease of childhood. Untreated maternal dental disease nearly

Paul Pholeros and his colleagues have been working for decades on improving health by improving the living environment and housing of Indigenous people in Australia. This successful model is now spreading to other continents. Ever since I watched this TEDx Talk, I have been wondering how we, dentists could apply similar thinking to improve health
© 2012-2024 All Rights Reserved